It will soon be two years since the virus known as COVID-19 started to roam around the world. The sad toll of this disease—over 5 million victims worldwide—is still incomplete, because we are far from seeing an end to the pandemic. It has been the largest public health crisis in the last century.
In the following lines I will try to review some of the COVID-19 complications and risks, which I will divide into two categories: complications that occur during while someone is infected, and complications that occur after the acute phase of the infection has passed (what we know now as “long COVID”).
One of the reasons why a SARS-CoV-2 infection is so feared is the extreme variety of clinical scenarios that patients experience, from asymptomatic infections (i.e. people experiencing no symptoms) in approximately 33% of cases, to severe cases, with pneumonia, in 14% of those infected, and very severe cases, which cause shock, respiratory failure or multiple organ dysfunction, in about 5% of cases. In the rest of the symptomatic cases (about 80%), the disease has a mild clinical picture, manifesting itself as a cold.
COVID-19 complications in the acute period of infection
1. Acute respiratory distress syndrome (ARDS)
ARDS is the main complication in patients who develop a severe form of COVID-19. This syndrome is an inflammation that affects both lungs. Many of these patients need artificial ventilation, and a third of them die. Another possible scenario is bacterial superinfection, in the context of weakened immune resistance and mucosal lesions caused by the SARS-CoV-2 infection.
These patients may develop septic shock, which is a widespread infection of the body, often ending in death. ARDS is associated with blood clotting disorders, which can also be lethal when out of control, and take the form of generalized microvascular thrombosis (i.e. the formation of blood clots in small blood vessels throughout the body). Surviving patients often experience long-term respiratory difficulties caused by the scarring of their lung tissue.
2. Cardiovascular complications.
These include:
- Myocarditis and pericarditis: These are inflammatory conditions of the heart muscle (myocarditis) or its protective sac (pericarditis). According to a study conducted on 1,597 US athletes who were infected with the coronavirus, 2.3% of them developed myocarditis. Fortunately, only a quarter of them had more serious forms of myocarditis.
- Stress cardiomyopathy, or broken heart syndrome: The heart function temporarily but significantly decreases due to enormous stress caused by the infection with the SARS-CoV-2 virus.
- Heart attack: It can occur as a complication of COVID-19 either in the context of pre-existing coronary heart disease or, indirectly, because the heart muscle is deprived of oxygen as a result of the respiratory complications mentioned above.
- Heart failure, especially acute right ventricular failure: This is another common complication.
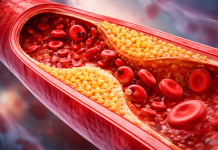
- Vascular thrombosis: Venous thromboembolisms (i.e. the formation of blood clots in the deep veins of the legs) or pulmonary embolisms (the formation and storage of blood clots in the lung’s arteries) are common in more severe forms of COVID-19, especially among patients who are treated in intensive care units, where their incidence can reach 40%. However, arterial thrombosis (blood clots in the arteries) can also occur, resulting in strokes even in patients under 50 years old who do not have major risk factors. For instance, according to a retrospective study conducted in several hospitals in New York, approximately 1.6% of adults who ended up in the emergency room due to COVID-19 suffered a stroke.
3. Neurological complications:
- Encephalopathy (a term referring to a brain condition): It is a common complication of COVID-19, especially among patients with severe infections. According to some studies, a third of these patients suffer from encephalopathy.
- Dizziness, strokes (see above), motor disorders, headaches, and sensory disturbances, such as loss of taste and smell, are also common, and can last for long periods.
4. Inflammatory complications:
COVID-19 is by definition an inflammatory condition, and more severe forms are characterized by an exacerbated inflammatory reaction, with increased fever and marked increase in substances that cause and increase the inflammatory immune response.
- The Guillain-Barré Syndrome: It is a rare autoimmune inflammatory neurological complication that can occur 5-10 days after the onset of COVID-19 and which affects the peripheral nerves.[1]
- Multisystem inflammatory syndrome in children (PIMS or MIS-C): This is a new, fortunately rare condition that occurs a few weeks after a child or young person has gone through COVID-19. It causes inflammation throughout the body and usually requires hospital treatment. Even less often, this syndrome can also occur in adults.
Post-COVID-19 complications
If, as I said earlier, acute complications of the SARS-CoV-2 virus infection occur in the vast majority of severe disease cases, long-term complications can occur regardless of the severity of the initial infection.
This category includes a variety of symptoms and health disorders, which persist for weeks and months after recovering from the acute phase of COVID-19. Many of these conditions have been grouped under the term “long COVID”. It is estimated that this syndrome affects approximately 10% of those in the 18-49 age group and 22% of those over the age of 70 who have experienced the SARS-CoV-2 infection.
Long-COVID syndrome
The most common symptoms of people suffering from the long COVID are: fatigue, difficulty concentrating or brain fog, difficulty breathing, coughing, diarrhoea, joint pain, chest pain, memory, concentration or sleep problems, muscular pain, headaches, palpitations, loss of smell or taste, depression or anxiety, fever, and dizziness. Often, these symptoms are aggravated by physical or mental activities. To be classified as the long COVID syndrome, these symptoms must be present 4 or 6 weeks after infection. We do not yet know the cause (or causes) of long COVID.
It is important to remember that this syndrome can also affect children and is one of the important reasons why parents should take this disease seriously and vaccinate their children, when recommended by a paediatrician.
I would like to end with the story of a co-worker who suffers from long COVID. He is a 45-year-old doctor who got infected with COVID-19 in December 2020, just 2-3 days before he managed to get vaccinated. Before COVID he was a very physically active person, full of energy, very loved by his patients, and a father of four children.
After developing COVID, he was left with persistent muscle pain and headaches, fatigue, and general malaise after minor physical exercises.
Before COVID-19, he did 50 push-ups 3 times a day, among other things. Now, he doesn’t even try, because he feels that he is not up for anything for 2-3 days if he does 10 push-ups. He was vaccinated after 3 months, hoping that the vaccine will help him (according to some estimates, vaccination leads to the resolution of this syndrome in about a third of cases), but it was all for nothing. He had to start working part-time and the most depressing part for him is that he does not yet see an improvement.
Gily Ionescu, MS, MD is MD is Board Certified in Internal Medicine and an infectionist at Walla Walla Clinic, Washington, SUA, and a member of the American College of Physicians.